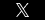The recent outbreak of fungal meningitis has many in the medical community desperate to get to the bottom of the cause. Possibilities abound and everyone appears to have a theory. Could it have been some moldy ceiling tiles? What about the dirty shoes of a careless employee? How about a contaminated ingredient?
The recent outbreak of fungal meningitis has many in the medical community desperate to get to the bottom of the cause. Possibilities abound and everyone appears to have a theory. Could it have been some moldy ceiling tiles? What about the dirty shoes of a careless employee? How about a contaminated ingredient?
There are many ways the fungus could have gotten inside the New England Compounding Center, a pharmacy in Massachusetts that has been blamed for the outbreak. The steroid injections made by the compounding pharmacy have already been recalled after leading to the death of 28 people and sickness in nearly 363 more (http://health.usnews.com/health-news/news/articles/2012/10/30/fungal-meningitis-outbreak-toll-now-28-dead-363-sickened).
So far regulators from both state and federal agencies have been quiet about what problem may have led to the contamination. It has been revealed that inspectors found fungus growing in more than 50 vials from the pharmacy. FDA investigators remain on the scene in Farmingham, Massachusetts in an attempt to better understand what went wrong.
Despite the lack of information, outside experts tend to agree that dirty conditions in the plant are likely to blame. This could include a number of possible sources of contamination, including faulty sterilizing equipment, tainted ingredients or sloppiness on the part of employees.
One problem for the pharmacy is that the drug used in the steroid injection is made without preservatives meaning there is no additive that is able to kill germs lurking in the medicine. Given this lack of preservative, it’s critical that the drug be manufactured under incredibly sterile conditions.
Though compounding pharmacies aren’t as tightly regulated as major manufacturers, they are supposed to follow certain basic rules including cleaning the floors and all other surfaces daily, monitoring the air supply in “clean rooms” where the drugs are actually made, ensuring that employees wear gloves and gowns and testing samples from each lot. These rules of standard practice exist in the U.S. Pharmacopeia, a national standards book for compounding medicines that is written by a nonprofit scientific organization.
To make the steroid used in this case, a chemical powder from a supplier was mixed with a liquid, sterilized through heating, then pumped into vials. It’s possible that the powder was contaminated, either at the New England Compounding Center or another location. Given the vast amount of the medicine produced, the time it would take to make the batches might allow the medicine time to be contaminated. It’s also possible that if a worker took a break for coffee or to go to the bathroom that they could have hurried back into the lab without properly washing up, thus introducing contamination.
Though this event has received a significant amount of media attention, it’s important to note that it’s not as uncommon as many people would think. In fact, just last year there were three similar incidents. At least 33 patients came down with fungal eye infections linked to a compounding pharmacy in Florida; a dozen patients were blinded after an outbreak caused by another compounder in Florida; and nine people in Alabama died from taking IV nutritional supplements made by a compounder in that state.
If you, or someone you know, have any questions regarding personal injury claims, please feel free to contact the experienced Charlotte, North Carolina wrongful death attorneys at Arnold & Smith, PLLC for a free consultation. Call at 704-370-2828.
Source: “Dirty shoes? How did steroids get contaminated?,” by Mike Stobbe, published at Yahoo.com.
http://news.yahoo.com/dirty-shoes-did-steroids-contaminated-205320745.html
See Our Related Blog Posts:
Recent Article Questions Necessity of Many Tests Ordered By Doctors
 Charlotte Injury Lawyers Blog
Charlotte Injury Lawyers Blog